  
Manual techniques may assist in promoting proprioceptive inputs to the central nervous system, indirectly contributing to the observed improvement in body stability. Having determined improvement in the treatment group in stability and behavior measures, the authors concluded that OMTh in combination with traditional therapy may be of clinical benefit for patients with BPPV. Within the treatment group, there was a significant correlation between reduced swinging area and global DHI changes ( P=.02), functional DHI subscale changes scores ( P=.03), and physical DHI subscale variation scores ( P=.01). Regarding stabilometric assessment, the treatment group showed a significant decrease in velocity ( P=.007), swinging of area ( P=.006), and swinging on Y-axis-O ( P=.023) the only difference between groups for stabilometric assessment was area measure ( P=.02). Compared with the sham group, the treatment group also showed statistically significant DHI improvements in global ( P=.02), function ( P=.03), and physical ( P=.03) scores, but not emotional scores ( P=.62). The treatment group had significant improvement in global, physical, and functional emotional aspects of DHI from baseline to follow-up (all P<.001). Both the DHI and stabilometric assessments of all patients were taken before the first week and 1 week after the last intervention. The sham group underwent light touch over areas of dysfunction, 10 minutes for evaluation and 10 minutes for treatment. Patients in the treatment group underwent an objective osteopathic evaluation and received 3 weekly 20-minute OMT sessions consisting of articulatory and muscle energy techniques, fascial unwinding, balanced membranous tension, and high-velocity, low-amplitude to the thoracic and lumbar spine. After a baseline assessment consisting of a Dizziness Handicap Inventory (DHI) and stabilometric examination, patients were randomly assigned to a treatment group (n=20) or sham group (n=20). 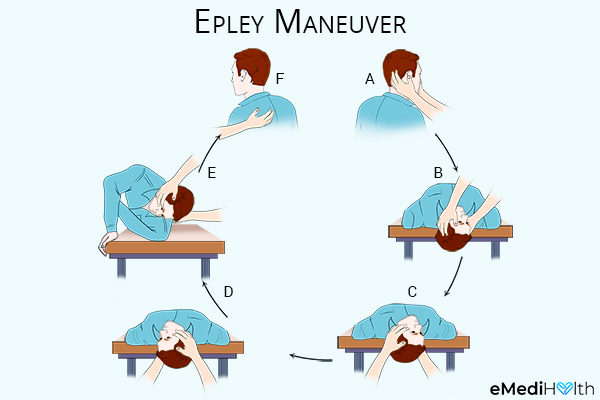
Patients were enrolled if they had dizziness 2 weeks after traditional clinical therapies. To determine the effectiveness of OMTh to relieve dizziness associated with BPPV, the researchers measured patient stability and assessed their behavior. 3 However, this study by Papa et al suggests that osteopathic manipulative therapy (OMTh manipulative care provided by foreign-trained osteopaths) could be helpful for managing refractory BPPV. 2 Refractory BPPV can be managed surgically. It is typically successfully managed using repositioning maneuvers (eg, Epley maneuvers, Semont maneuvers, home exercises) and sometimes with medication. Pathophysiologically, BPPV is associated with calcium debris in the semicircular canal. Benign paroxysmal positional vertigo (BPPV) is an episodic spinning sensation with head repositioning arising from dysfunction of the inner ear. In 2013, Fraix et al 1 reported that osteopathic manipulative treatment (OMT) for spinal somatic dysfunction improved balance in patients with chronic dizziness. Impact of osteopathic therapy on proprioceptive balance and quality of life in patients with dizziness. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
